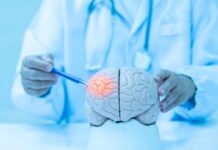
One daily glass of red wine might slash your heart disease risk by 25%, but it could also hike your cancer odds by 10%—a gamble few should take.
Story Snapshot
- French Paradox myth promised heart protection from wine, now debunked by modern science showing alcohol’s hidden harms.
- Moderate intake links to 13-26% fewer CVD events in some studies, yet raises breast cancer risk 5-10%.
- WHO declares no safe alcohol level; benefits overstated due to flawed data like sick quitter bias.
- Polyphenols offer promise, but alcohol’s effects on blood pressure and mortality tip scales against routine drinking.
French Paradox Origins and Rise
A 1991 CBS 60 Minutes segment spotlighted France’s low heart disease rates despite fatty diets, crediting red wine’s resveratrol and polyphenols. Observational studies in the 1990s and 2000s revealed a J-shaped curve: 1-2 drinks daily cut CVD mortality 18-23% compared to teetotalers. Researchers hailed antioxidants for boosting HDL cholesterol and insulin sensitivity. This narrative fueled wine’s health halo, especially in high-risk groups like type 2 diabetics.
Observational Wins Meet RCT Realities
Early data showed moderate wine (5-15g alcohol daily) tied to 26% lower CVD risk and 35% reduced mortality versus abstainers. RCTs in post-heart attack patients confirmed 13% fewer events (HR 0.87) with red wine polyphenols improving lipids and gut health. Type 2 diabetics saw 22% fewer CV incidents (aHR 0.78). Yet chronic trials exposed mixed results on hypertension and endothelial function. Alcohol raised endothelin-1, constricting vessels without regressing plaques.
Guideline Shifts and Cancer Warnings
WHO’s 2023 statement proclaimed no safe alcohol level, overturning pro-moderate claims. Dietary Guidelines for Americans capped intake at one drink for women, two for men, citing breast cancer risks. MD Anderson experts state even one glass daily elevates cancer odds. UC Davis notes 18-23% CVD death drops but 5-10% breast cancer hikes. Post-COVID scrutiny amplified these reversals, prioritizing absolute harms over relative gains. Abstinence advocacy gains traction among guideline setters.
Stakeholders clash: WHO, CDC, and DGA push public health via zero-alcohol pushes, while Mayo Clinic weighs alcohol’s heart role against outweighing risks. Researchers like Levantesi and Banach dissect polyphenols from ethanol. Wine promoters cling to health marketing, but academics via RCTs expose biases.
Expert Consensus on Net Harms
Stanford’s 2025 analysis rejects causal proof for heart or diabetes protection from moderate drinking. PMC reviews affirm antioxidant benefits but flag blood pressure elevations and null mortality effects. Blue Zone wine myths, like Sardinia’s, crumbled under meta-analyses showing no longevity boost. Limited long-term RCTs beyond two years leave uncertainties, yet confounders like ex-drinkers skewing abstainer data undermine J-curves. Polyphenol isolation emerges as future focus.
Women face heightened breast cancer risks; type 2 diabetics glean subset benefits. Public systems bear alcohol disease burdens. Wine sales may dip sans health halo, spurring non-alcoholic pivots. Social norms trend zero-proof; policies demand warning labels. Beverage research eyes polyphenol extraction sans ethanol.
Sources:
PMC narrative review on red wine and cardiovascular health
PMC review on wine polyphenols and vascular effects
UC Davis: Is wine really healthy? Experts summarize research
MD Anderson: Red wine and your health: Facts and myths
Stanford: Alcohol consumption and your health: What the science says
Mayo Clinic: Red wine and heart health